Article Categories
- All Categories
-
 Data Structure
Data Structure
-
 Networking
Networking
-
 RDBMS
RDBMS
-
 Operating System
Operating System
-
 Java
Java
-
 MS Excel
MS Excel
-
 iOS
iOS
-
 HTML
HTML
-
 CSS
CSS
-
 Android
Android
-
 Python
Python
-
 C Programming
C Programming
-
 C++
C++
-
 C#
C#
-
 MongoDB
MongoDB
-
 MySQL
MySQL
-
 Javascript
Javascript
-
 PHP
PHP
-
 Economics & Finance
Economics & Finance
Agglutination - Definition, Reactions, and Applications
Introduction
Agglutination is a type of antigen-antibody reaction where the antibody interacts with the particulate antigen which eventually gives us visible clumping. Here antigen is not soluble in the aqueous environment. Antibodies here are called agglutinins and antigens are called agglutinogens. Clumping is due to the cross-linking between a polyvalent antigen and agglutinins.
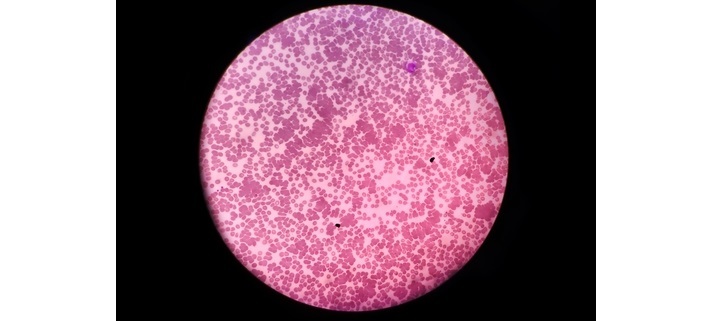
RBC Agglutination
Principle
Antigens involved in the agglutination reaction are surface antigens present on erythrocytes, bacterial particles or antigens attached to some matrix. These particles involved in agglutination reaction should have multiple binding sites to form cross links resulting in clumping.
To form a visible clumping in an agglutination reaction, both the antigens and antibodies should be in equal concentrations. If any one of the 2 components is at different concentrations, visible clumps are not formed.
Prozone Effect
Excess of antibodies or agglutinins causes the inhibition of agglutination reaction which is known as prozone effect.
This concept is also true for precipitation reactions. Prozone effect can be occurred due to the following reasons ?
-
When the antibodies concentration is more, the antibody binding sites are greater than the available epitopes on the antigen. This results in tnivalent binding where the cross-linking is not observed. Then the agglutination reaction is inhibited.
This can be diagnosed by varying the antibody concentrations for a given concentration of the antigen. Here the antibody levels are diluted from the higher concentrations to lower and a particular amount of antigens are added. In diluted concentrations of antibodies, when we add a particular amount of antigen, agglutination is observed whereas in the higher concentrations, agglutination is not seen.
-
Prozone effect can also occur because of polyclonal antibodies (where different types of antigens bind to different epitopes). IgG, IgM, etc., can be used as polyclonal antibodies. Here when polyclonal antibodies are used for reactions, IgG binds to the antigen but it cannot cause agglutination.
Such antibodies are termed incomplete antibodies and they block the binding of IgM antibodies to the antigen. This may be due to 2 main reasons.

IgM antibody pentamer molecule
Due to the restricted flexibility in the hinge regions of the IgG antibody these cannot bind properly to the epitope of an antigen.
Density or distribution of epitopes within the antigens may be present in deeper pockets hence inhibiting the agglutination reaction.
Agglutination occurs in the two stages
Sensitization Stage ? antibodies bind to a single epitope of an antigen.
Lattice Forming Stage ? The 2 antigen binding sites on a single antibody binds to epitopes of 2 different antigens. This causes the cross-linking of antigen particles resulting in the formation of lattices.
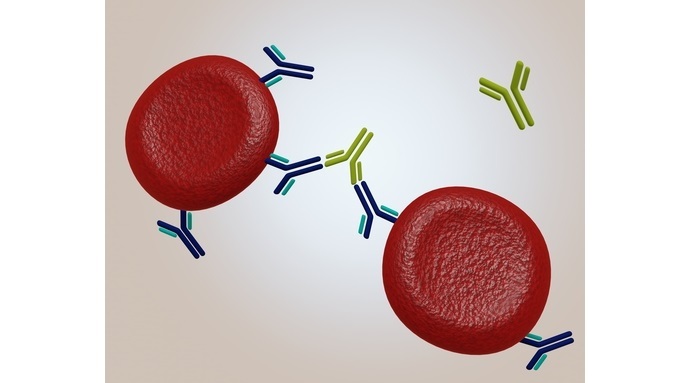
The formation of a bridge between red blood cells that have IgG bound
Factors That Influence the Agglutination Reactions
Some of the factors that influence the agglutination reactions are ?
pH ? Agglutination reaction works best around pH 6.5-7.5. pH below 5 and above 8 are not favorable for agglutination as the antibodies get precipitated at this pH.
Ionic Strength of a Solution ? Most of the agglutination reactions occur in saline. However, some reactions are favorable at low ionic strength solutions. Low ionic strength solutions of about 0.03 mol/L NaCl in sodium glycinate solution are normally used in blood banks for agglutination assays
Temperature ? for IgG, lattice formation is favorable between temperatures 30O-37O. For IgM it is 4O-27O.
Some of the factors which enhance the agglutination reactions are viscosity, enzymes, agitation or centrifugation, etc.
Viscosity ? Agents like dextran and polyethylene glycol increases the viscosity reducing the water present around the antibodies and antigens resulting in the enhancement of binding between them and lattice formation.
Enzymes ? Enzymes like bromelin, trypsin, and papain reduce the charge on particles and also reduce the water enhancing the lattice formation and agglutination.
Physical Methods ? Methods like centrifugation increases the contact between cells and enhances agglutination.
Applications
In diagnostic immunology, agglutination reactions have a wide variety of applications.
It is used to determine both antigens and antibodies in serum and other fluids.
Serologic Test
Most importantly agglutination reactions are routinely performed in the blood banks to determine ABO and Rh blood typing in preparations for transfusions.
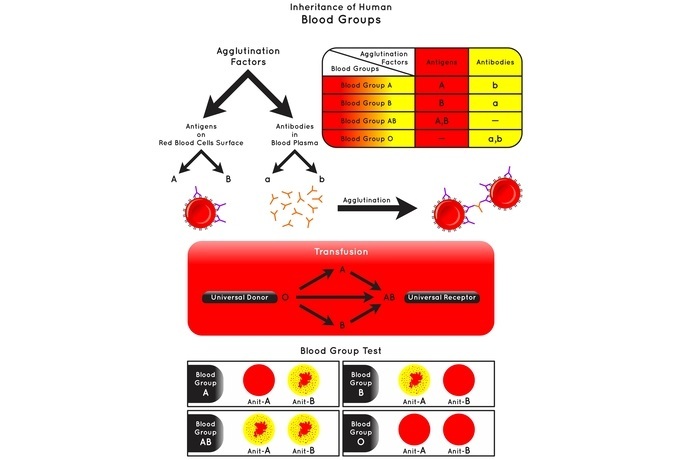
Coomb?s test for anti-Rh antibodies.
Widal test for typhoid.
Detection of illicit drugs like cocaine, heroin, etc.
Measurement of therapeutic drugs, hormones and plasma protein levels in blood.
Stereotyping of bacteria, parasites etc.
Diagnosis of infectious antigens like bacteria, virus etc.
Types of Agglutination Reactions
Agglutination reactions are classified into 2 types based on whether the antigenic determinants or epitopes to which antibodies are bind or present naturally on the target cells or particles or not. They are ?
Active Agglutination or Direct Agglutination
Here the epitopes of interest are present naturally on the test particles. For example, antigens present on RBCs, antigenic determinants or antigens present on bacterial and fungal cells etc.
Antibodies combine directly with this antigen and result in agglutination.
When a bacterial suspension is placed on the glass slide and added with the antiserum containing the antibodies specific to these bacteria, it results in the clumping clearing the suspension which indicates that the agglutination has occurred and the test is positive.
Applications
These types of bacterial agglutination tests are routinely used for the identification of bacterial isolates from the clinical specimen.
These are also used for blood typing and cross-matching before blood transfusions.
Other applications include the Widal test for diagnosis of typhoid fever, Brucella agglutination test for Brucellosis and Wein Felix test for Rickettsiosis.
Passive Agglutination or Indirect Agglutination
Here the epitopes of interest do not occur naturally on the cells or particles to be agglutinated.
In these cases, the epitopes or soluble antigens are chemically fixed to carrier particles. Examples of carrier particles are latex, polystyrene, bentonite etc.
Earlier RBCs were used for passive agglutination but synthetic carrier particles provide advantage of uniformity, stability and consistently hence they are preferred now. This method is known as reverse passive agglutination.
Advantage of this agglutination is that it ca be easily performed and interpret results in cases where pathogen culture is not feasible or only soluble antigens are available. For example, in viral diseases
Here the soluble antigens are chemically fixed to the latex beads. Once the carrier particles are coated with the antigens, antibodies specific to these antigens are added. These antibodies react with the antigens and particles agglutinate with one another.
We can also detect the antigens by reversing the process that is instead of coating with carriers, these antigens are coated with the antibodies.
Applications
These are used for diagnosing various bacterial and viral diseases. Example is latex agglutination test for Rubella antibody testing.
Conclusion
When a particulate antigen (cells that carry antigenic molecules on their surface) binds to the specific antibodies, cross linking occurs which results in visible clumping or agglutination. Here the clumping is visible to the naked eye. Here these particulate antigens are insoluble molecules.
Like precipitation reactions, agglutination occurs when there are equal proportions of antigen and antibodies. Direct and indirect agglutinations are the 2 types which have wide range of applications in the diagnostic immunology.


